Abstract
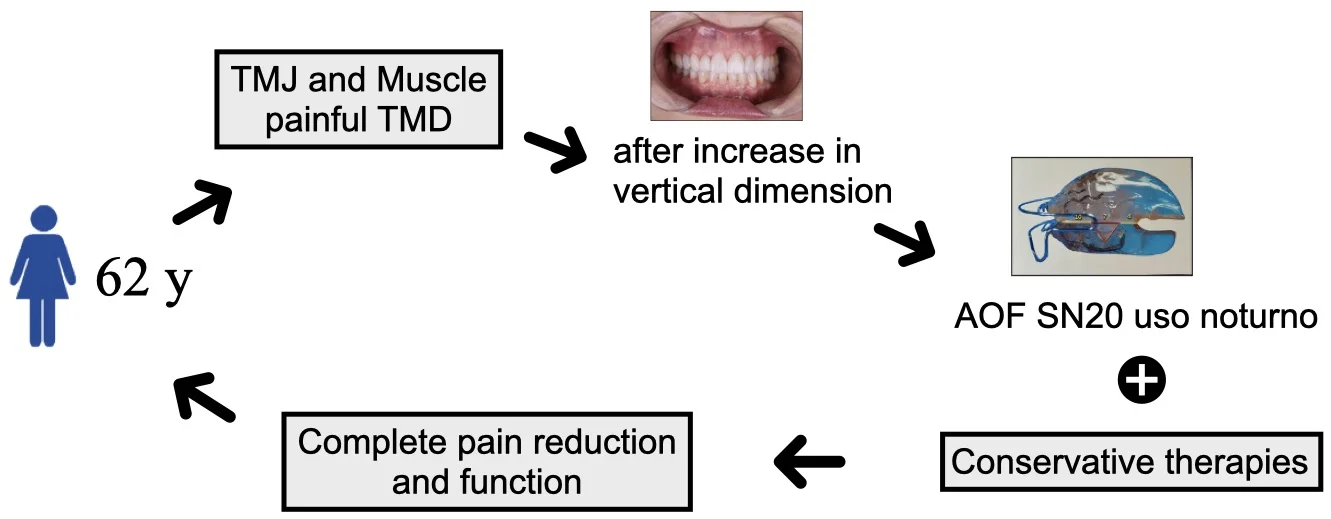
The literature indicates that patients with a history of Temporomandibular Disorder (TMD), who experience sudden occlusal changes, may worsen their parafunctional habits and develop TMD again. In this sense, the aim of this study is to present a clinical case of recurrent chronic TMD after oral rehabilitation (increase of vertical dimension in all teeth) using Simões Network 20 (SN20) functional orthopedic appliance as one of the resources therapies. The patient was female, 62 years old, and complained of disabling pain, anxiety symptoms, hypervigilant and history of TMD. The patient reported failure of other treatment modalities, including use of the smooth stabilizer device. The diagnosis was chronic TMD – primary osteoarthritis of the temporomandibular joint and related myofascial pain and orofacial migraine. Treatment included physical measurements, instructions, peripheral and central medication, AOF type SN20 (night use). After three months of therapy, the patient showed significant improvement with complete pain reduction. The use of the AOF SN20 together with conservative measures represents a valuable therapeutic modality for patients with chronic TMD.
Highlights
- Previous TMD patients who have experienced sudden occlusal changes may develop TMD again.
- This paper presents a clinical case of recurrent chronic TMD.
- There was complete pain reduction using the AOF SN20 along with conservative therapies.
1. Introduction
Temporomandibular disorder (TMD) groups a set of clinical conditions affecting the masticatory muscles, temporomandibu-lar joint (TMJ) and all associated tissues. The most common symptom is pain, usually localized to the muscles of mastication and/or the preauricular area. Chewing and other mandibular functions aggravate the pain. In addition to these symptoms, patients often report restricted mouth opening and temporomandibular joint noises. These complaints make TMD the second reason for treatment in the dental practice [1].
Patients with pathological or severe tooth wear, either by chemical or mechanical cause, may need restorative care to compensate for the loss of tooth tissue, possibly comprising full rehabilitation at an increased vertical dimension of occlusion (VDO). [2] However, several studies show that patients with a history of TMD, who experience sudden occlusal changes, may worsen their parafunctional habits and develop TMD again. [3, 4] Based on this, the aim of this study is to present a clinical case repot of recurrent chronic TMD after oral rehabilitation (increase in vertical dimension in all teeth), in a patient with a history of TMD, hypervigilant, with symptoms of anxiety who used the Simões Network 20 (SN20) functional orthopedic appliance as one of resources therapies.
2. Methods
Case Report: A woman, 62 years old, complained of disabling pain – Visual Analogue Scale (VAS) 10, beginning after oral rehabilitation - increase in vertical dimension in all teeth (Figs. 1, 2). The pain was constant, worsening with function, localized to the left temporomandibular joint, the temporal region and the teeth on the right side.
Fig. 1Before rehabilitation
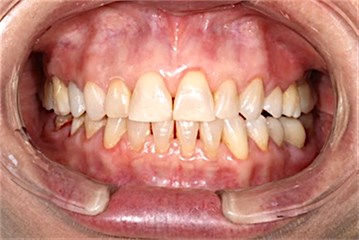
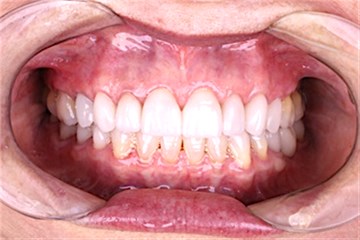
Fig. 2Post rehabilitation
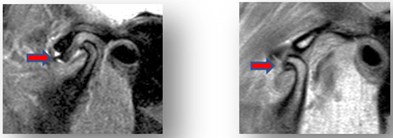
TMJ Magnetic Resonance Imaging (MRI) showed disc displacement with reduction on the right side (Fig. 3). On the left side effusion, spinal edema and disc displacement without reduction (Fig. 4).
Fig. 3MRI right side TMJ before treatment
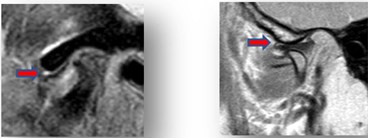
Fig. 4MRI left side TMJ before treatment
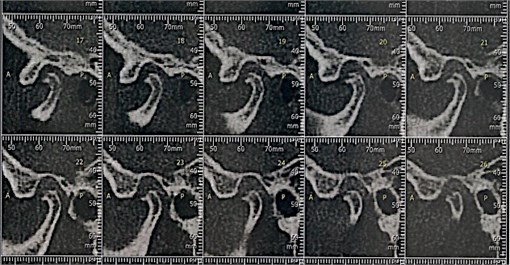
Computed tomography showed upper slope planning on the right side (Fig. 5) and morphological changes on the left side, erosion and flattening in the upper slope of the mandible, osteophyte in the anterior region (Fig. 6). The patient reported failure of other treatment modalities, including use of the smooth stabilizer device.
Fig. 5TC right side TMJ before treatment
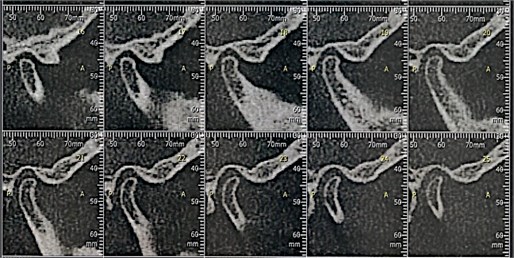
Fig. 6TC left side TMJ before treatment
3. Result and discussion
Diagnosis: Chronic DTM – temporomandibular joint disorder (primary osteoarthritis), myofascial pain with reference and orofacial migraine.
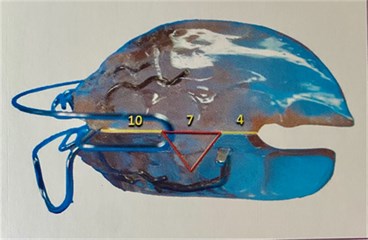
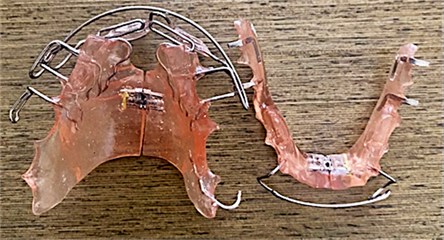
Treatment: Placement of the functional orthopedic device (AOF) type SN20 night use. The SN20 is a cusp-fossa compliant bioplastic device, whose excitation response is exerted through minimal alternation of muscle contraction [5, 6] (Fig. 7). Physical therapies (thermotherapy, massage, jaw exercises), instructions, peripheral drugs (non-steroidal anti-inflammatory – AINES) and central medication (tricyclic antidepressant), laser therapy, TENS were used as further conservative therapies.
After three months of therapy, the patient showed significant improvement with complete pain reduction and function.
Further studies are needed with samples that include comparison groups for the treatment of chronic TMD with the use of the functional orthopedic device and the conservative therapies versus patients who only used the conservative therapies. Further-more, more robust sampling is a recommended strategy for increasing the credibility of this result.
Fig. 7Functional orthopedic appliance SN20
4. Conclusions
The use of the AOF SN20 along with conservative therapeutic procedures represents a valuable therapeutic modality for patients with chronic TMD. However, randomized clinical trials are needed to demonstrate the contribution of OFM to the treatment of TMD.
References
-
R. Leeuw, Dor Orofacial: Guia De Avaliação, Diagnóstico E Tratamento. São Paulo: Quintessence, 2010.
-
B. A. C. Loomans et al., “Clinical performance of full rehabilitations with direct composite in severe tooth wear patients: 3.5 Years results,” Journal of Dentistry, Vol. 70, pp. 97–103, Mar. 2018, https://doi.org/10.1016/j.jdent.2018.01.001
-
P. M. Niemi, Y. Le Bell, M. Kylmälä, T. Jämsä, and P. Alanen, “Psychological factors and responses to artificial interferences in subjects with and without a history of temporomandibular disorders,” Acta Odontologica Scandinavica, Vol. 64, No. 5, pp. 300–305, Jan. 2006, https://doi.org/10.1080/00016350600825344
-
B. Imhoff et al., “Occlusal dysesthesia-A clinical guideline,” Journal of Oral Rehabilitation, Vol. 47, No. 5, pp. 651–658, May 2020, https://doi.org/10.1111/joor.12950
-
Simões Wa. In: Simões Wa et al., “Ortopedia Funcional: Fundamentos e Atualização,” in Ortopedia Funcional dos Maxilares, DTM e Dor Orofacial Jaw Funcional Orthopedics, TMD and Orofacial, Ribeirão Preto, SP, 2013.
-
D. H. A. Cardoso et al., “OFM na Dentição Permanente,” in Pesquisa e Excelência Clínica. Coletania CIOSP, Nova Odessa.
About this article
The authors have not disclosed any funding.
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
The authors declare that they have no conflict of interest.
The research met all applicable standards for the ethics of experimentation. Participants provided written informed consent prior to the study.
