Abstract
Introduction: Postural stability can be maintained in balance by muscle tone [1]. Change in the mandibular position or posture, may have influence in the postural reflex, defined as an involuntary defense movement [2] to correct deviations and keep the body in balance. If the postural change is constant, the muscles will move the mandible to a more comfortable position, with consequent postural change2 and plantar support. The aim of the study was to compare the plantar support in centralized and in lateralization mandibular position in seven years’ children. Main text: This study was approved by research ethics committee (No. 4.346.542). A pilot study was carried out with seven-year-old children of both sexes. Photogrammetry was performed with spherical markers in the region of the right tragus and chin symphysis (Fig. 1) concomitantly with baropodometry following (Fig. 2, 3) the protocol established by Bittar et al. [4]. Analysis of mandibular displacement and plantar support were performed with centralized mandibular position (maximum intercuspation) and with lateral displacement to the right and left. Statistical analysis compared the differences in mandibular displacement to the right and left sides using Student’s test. Differences in plantar support variables with centralized mandibular position and in right and left lateralization position were established by the Anova one way test and the Bonferroni pos test. Significant statistical difference was reached by 5 %. Results: Twelve seven-year-old children were included, 20.8 (3.25) Kg and 1.18 (0.06) meters. The sample present greater lateral displacement of the mandible to the lefts compared to right side. Mandibular lateralization was confirmed with statistical difference compared to mandibular position centralized. No difference in all plantar support variables was observed between the three positions: centralized and left and right lateralization. Conclusions: No differences were observed for plantar support compared position in mandibular lateralization and centralized position. Mandibular lateralization displacements did not change plantar support.
1. Introduction
Postural stability can be maintained in balance by muscle tone [5]. If there is a change in the mandibular position or posture, these can trigger the postural reflex, which is an involuntary defense movement [6] to correct deviations and keep the body in balance. The more balanced the afferents from the visual, vestibular and somatosensory systems, the more difficult it is to observe changes in the stomatognathic system with plantar support [2]. The aim of the present study was to determine whether different mandibular positions alter plantar support in seven-year-old children. The impact and differences of mandibular position with plantar support are inconclusive. Researches present inadequate methodologies with methodological bias and small samples. In this way, studies with a larger sample size may contribute to establish the influence of mandibular positioning on plantar support and guide clinical assessment and rehabilitation strategies in children.
2. Study
Pilot study with a sample of 12 children, both sexes, 7 years old, weighing 20.8 (3.25) and height 1.18 (0.06 s). Project approved by the Research Ethics Committee of the University State of Londrina, with opinion No. 4,346,542.
Markers were placed at the points: right tragus, chin and left tragus regions (Fig. 1) for photogrammetry. To confirm the lateral displacement of the mandible, the mento-tragus distances to the right (A), PIM (B) and left (C) were considered, with analysis of the displacement in mm using the IMAGEJ program.
Baropodometer for plantar support following protocol [4] (Fig. 2). Plantar support variables: Mean pressure, maximum pressure and surface area in the right and left foot (Fig. 3), analyzed by BaroScan.
Statistical analysis compared differences in mandibular displacement to the right and left by Student’s test. Differences in plantar support variables with the mandible in the central position, displaced to the right and to the left were established by the Anova one way test and the Bonferroni post test. The significant difference was set at 5 %.
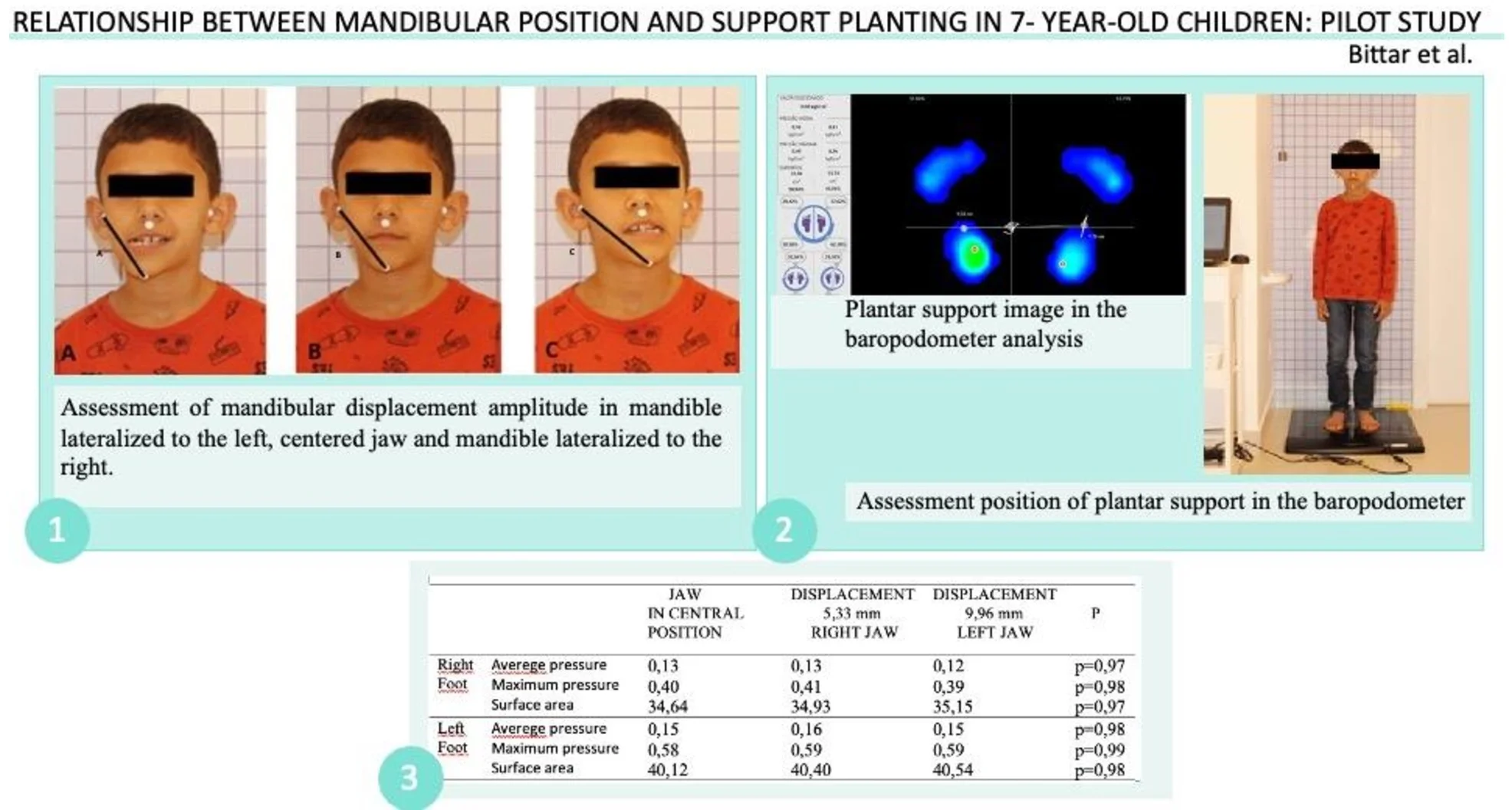
Fig. 1Assessment of mandibular displacement amplitude in centralized posture and in right and left lateralization: a) mandible lateralized to the right, b) centered jaw, c) mandible lateralized to the left
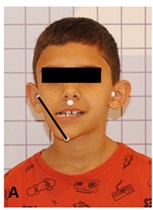
a)
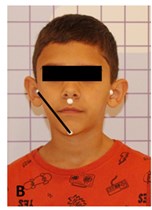
b)
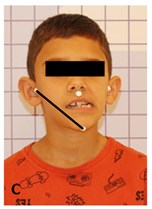
c)
Fig. 2Assessment position of plantar support in the baropodometer

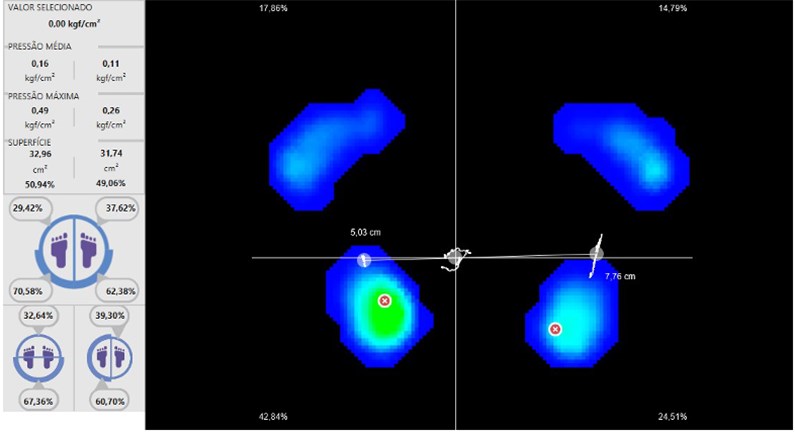
Fig. 3Plantar support image in the baropodometer analysis, average pressure, maximum pressure and surface area
3. Results
The displacement distance of the mandible to the right was 5.33 mm and to the left was 9.96 mm, with a significant difference ( 0.01).
Table 1Results
Jaw in central position | Displacement 5,33 mm Right jaw | Displacement 9,96 mm left jaw | |||
Right foot | Averege pressure Maximum pressure Surface area | 0,13 0,40 34,64 | 0,13 0,41 34,93 | 0,12 0,39 35,15 | 0,97 0,98 0,97 |
Left foot | Averege pressure Maximum pressure Surface area | 0,15 0,58 40,12 | 0,16 0,59 40,40 | 0,15 0,59 40,54 | 0,98 0,99 0,98 |
4. Conclusions
Children in this study have greater left-sided jaw movement. Mandibular movements did not change plantar support. Research with a larger must be performed to actually prove or disprove these results.
References
-
A. T. Masi and J. C. Hannon, “Human resting muscle tone (HRMT): Narrative introduction and modern concepts,” Journal of Bodywork and Movement Therapies, Vol. 12, No. 4, pp. 320–332, Oct. 2008, https://doi.org/10.1016/j.jbmt.2008.05.007
-
W. C. Ober, C. W. Garrison, and A. C. Silverthon, Fisologia, un approccio integrato. Casa Editrice Ambrosiana, 2000.
-
S. Julià-Sánchez, J. Álvarez-Herms, and M. Burtscher, “Dental occlusion and body balance: A question of environmental constraints?,” Journal of Oral Rehabilitation, Vol. 46, No. 4, pp. 388–397, Apr. 2019, https://doi.org/10.1111/joor.12767
-
K. C. B. Bittar, S. S. I. Oliveira, M. C. B. Michel, S. P. Terçarolli, C. L. Zamboti, and C. S. G. Macedo, “Reliability of plantar pressure and postural control measures of children from 4 to 12 years: analysis by baropodometry,” Motriz: Revista de Educação Física, Vol. 26, No. 3, 2020, https://doi.org/10.1590/s1980-6574202000030002
-
A. S. Pollock, B. R. Durward, P. J. Rowe, and J. P. Paul, “What is balance?,” Clinical Rehabilitation, Vol. 14, No. 4, pp. 402–406, Aug. 2000, https://doi.org/https://doi.org/10.1191/0269215500cr342oa
-
A. Cuccia and C. Caradonna, “The Relationship Between the Stomatognathic System and Body Posture,” Clinics, Vol. 64, No. 1, pp. 61–66, Jan. 2009, https://doi.org/10.1590/s1807-59322009000100011
About this article
Special thanks to my advisor Dr. Christiane Guerino Macedo for sparing efforts in all my dissertation work and Camille Ludovico for all the attention in refining my writing. I thank Dra. Patrícia Valério therefore taught in the physiology of the stomatognathic system. It was essential for me to be able to link my work.
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
The authors declare that they have no conflict of interest.
The research met all applicable standards for the ethics of experimentation. Permission to carry out biomedical research was granted by CAAE of Universidade Estadual de Londrina, No. 37725020.8.0000.5231 permission number 4,346,542, issue date October 19, 2020. Participants provided written informed consent prior to the study.
